From patient information journey
to experience design in AMD & DME
Ux research – information design – service design
From information gaps to meaningful patient experience :
Rethinking the informational journey for AMD and DME patients
Date
– 2023
Client
– Roche with Vivio agency
Role
– Ux research
– mediation
– information design
– service design

When someone is diagnosed with Age-Related Macular Degeneration (AMD) or Diabetic Macular Edema (DME), the first impact isn’t only physical, it’s psychological.
Yet most patients say they are “satisfied” with the information they receive. That contradiction became the starting point of this research.
This project aimed to explore how patients diagnosed with Age-Related Macular Degeneration (AMD) and Diabetic Macular Edema (DME) search for and access information about their disease and its management, and how this informational journey could be transformed into a more effective and supportive experience.
The ambition was clear: move from fragmented information flows to a structured, patient-centered experience grounded in real usage behaviors. Because the risk was to build more content without understanding real behaviors.

We conducted a mixed-method study combining:
-
200 patients & 30 caregivers
-
Recruitment via 64 pharmacies
-
Supervision by a scientific committee and ophthalmology leaders
Through quantitative data and semi-structured interviews, we explored:
-
Information needs at diagnosis and over time
-
Trust in different information sources
-
Media and channel preferences
-
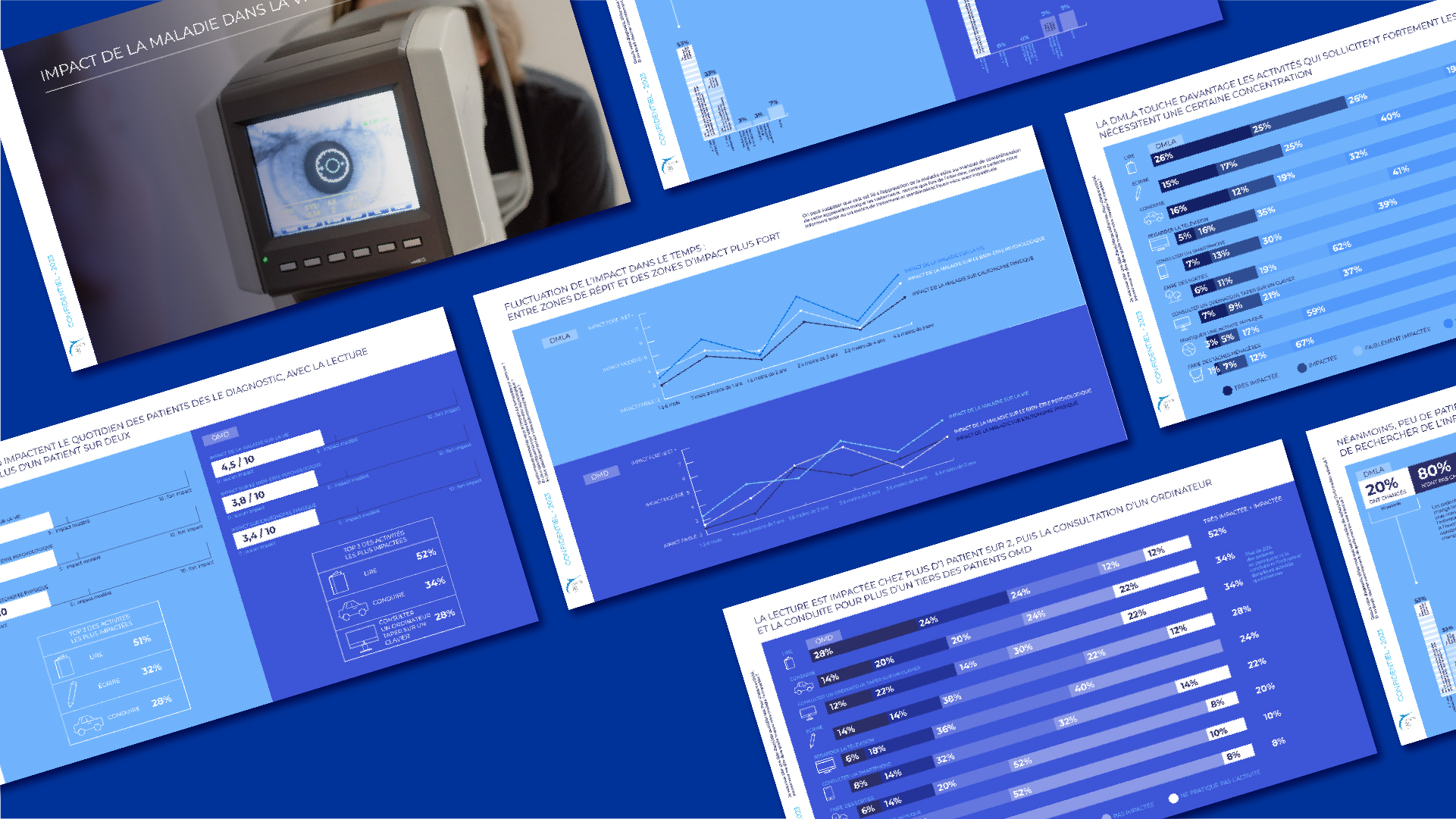
Emotional and functional impact of the disease
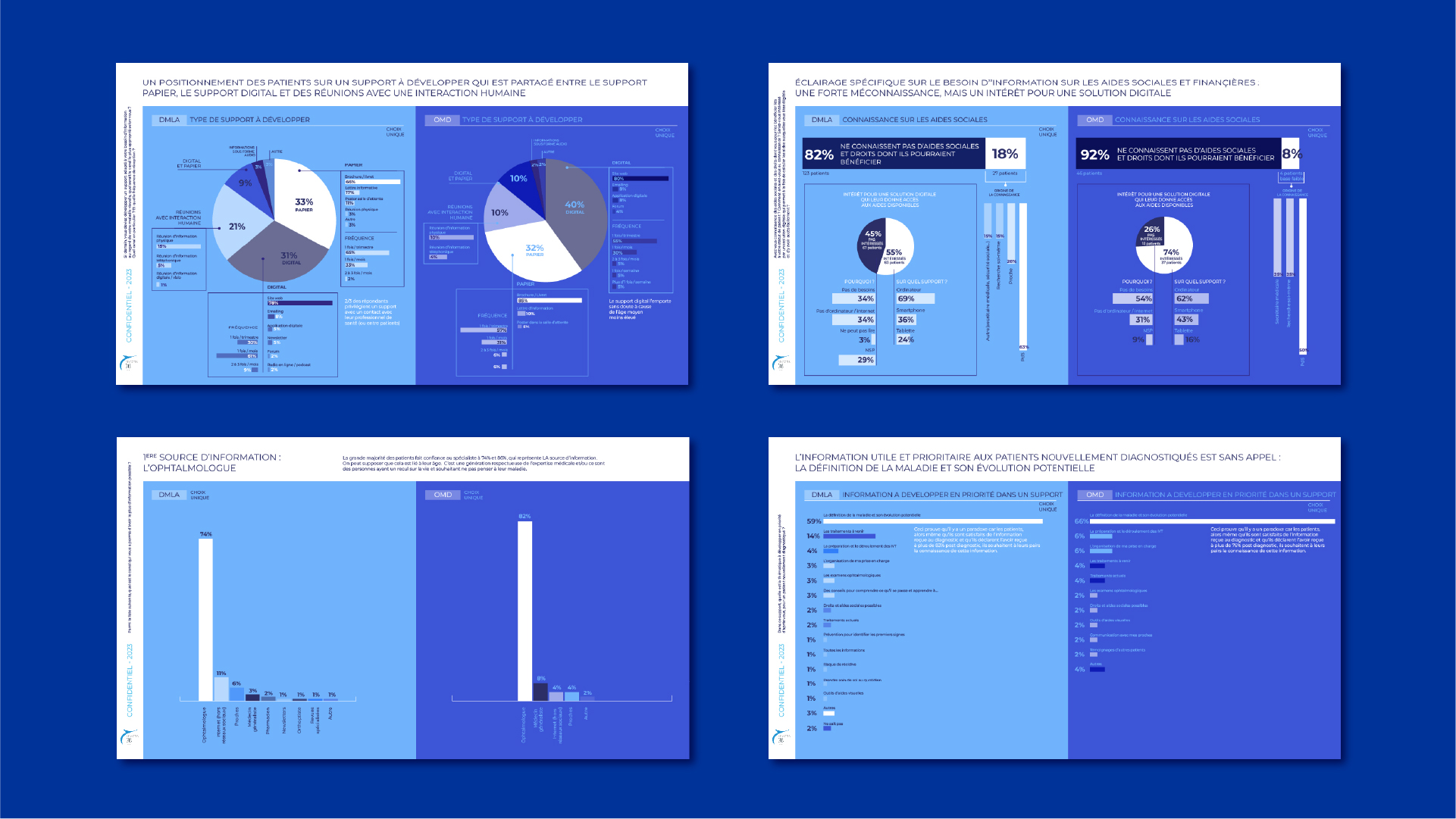
We discovers that most patients are passive information seekers.
They overwhelmingly trust their ophthalmologist (74–82%) and rarely search online.
A significant proportion does not use the internet daily.
Despite reporting high satisfaction levels, many patients:
-
Do not fully understand disease progression
-
Are unaware of recurrence risks
-
Experience psychological distress peaks months and years after diagnosis
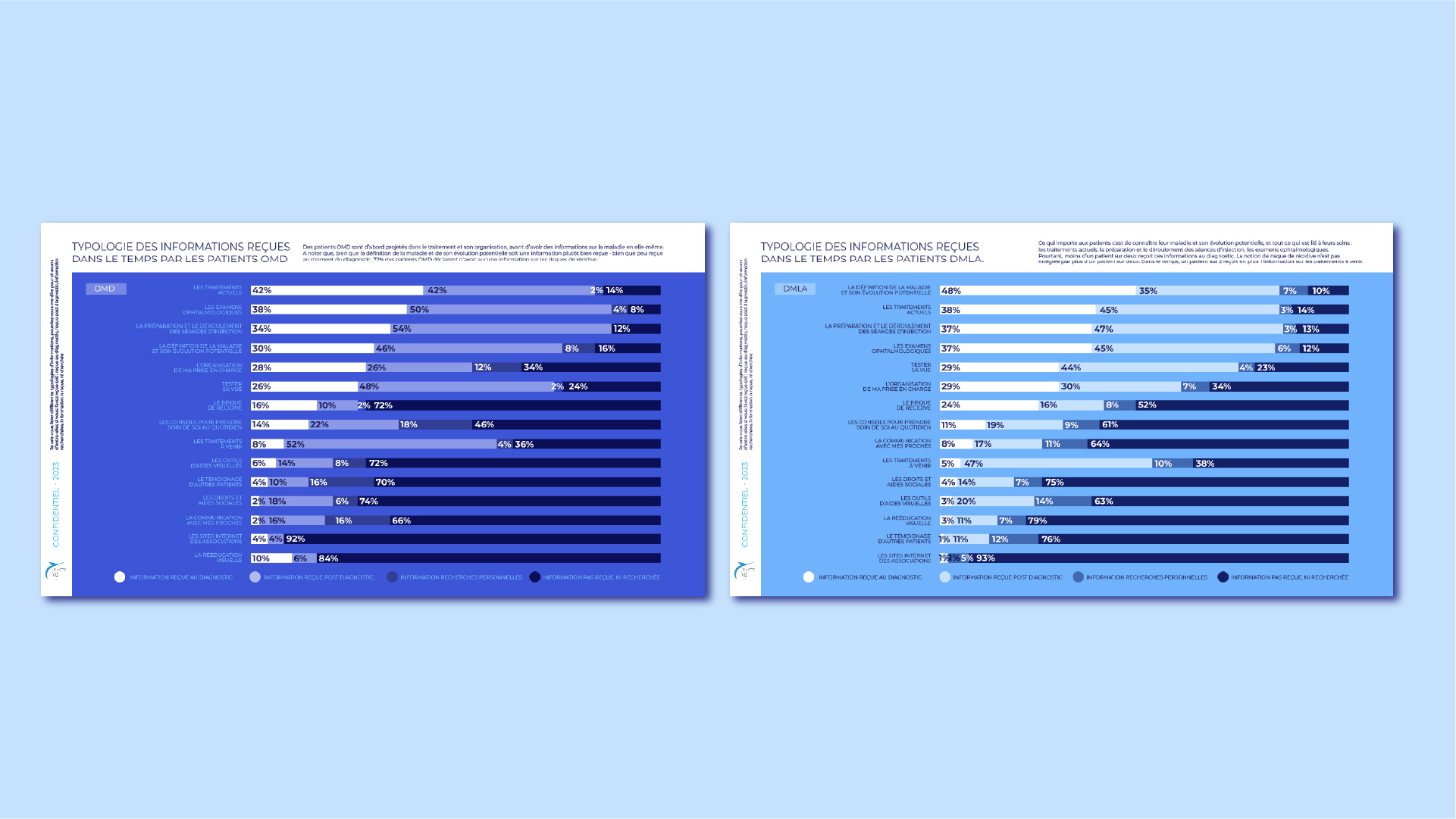
Information was delivered, but not fully integrated.
The issue wasn’t access to information. It was timing, sequencing, and emotional readiness.
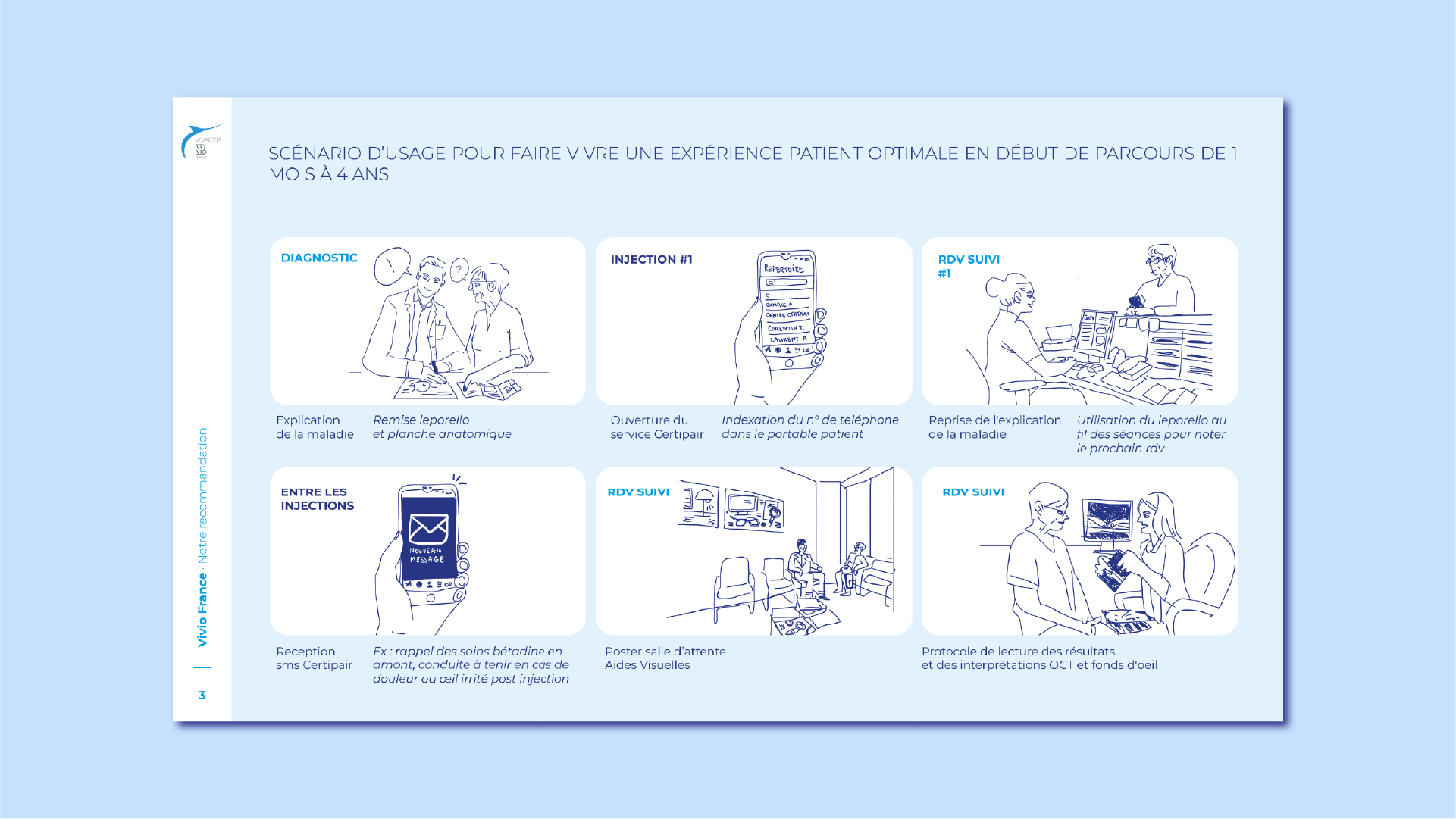
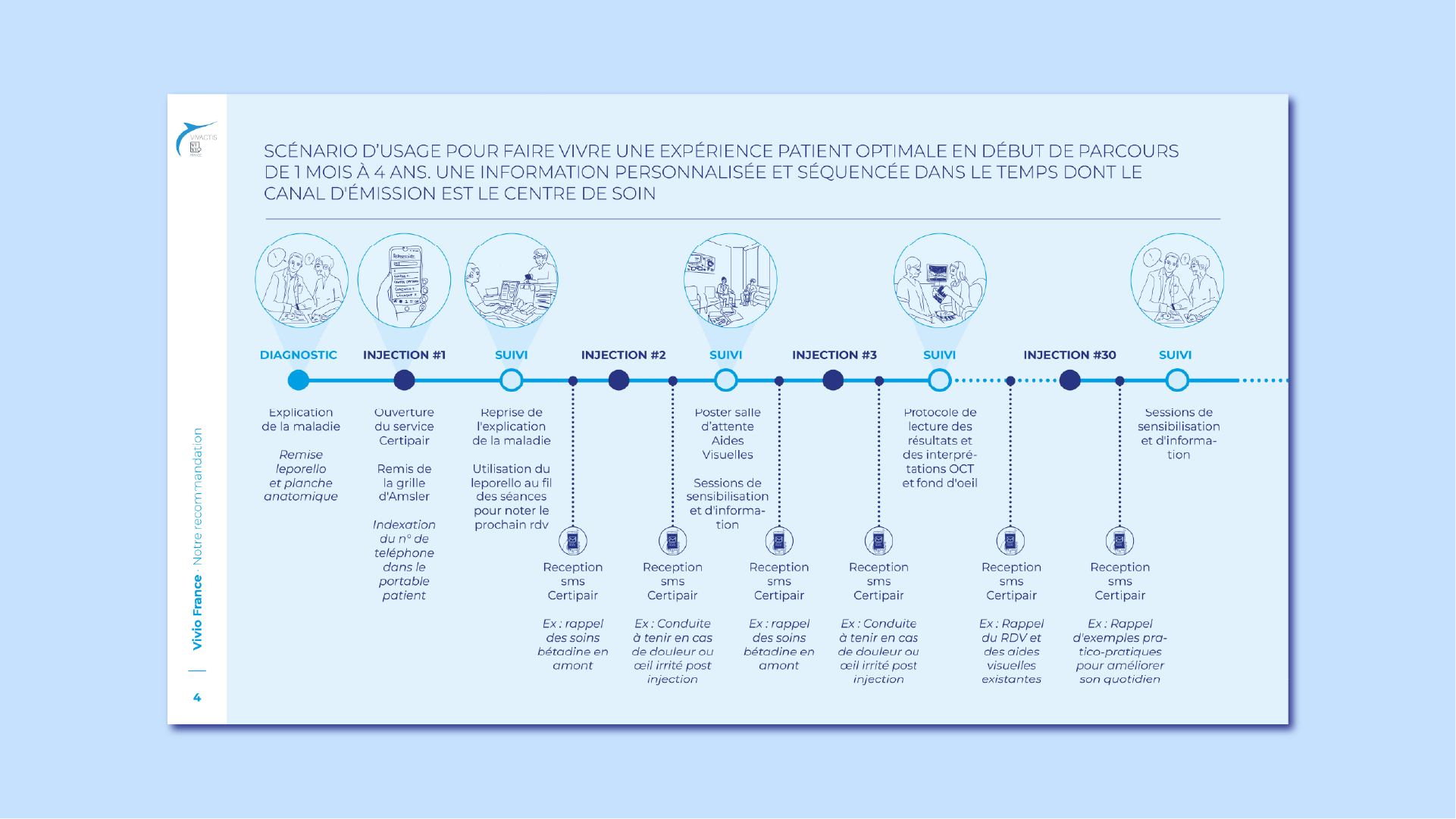
Patients needed structured, essential information at diagnosis, and progressive, supportive reminders at key moments in their journey. Not more content but a better orchestration.

The research led to a redesigned informational strategy built around:
-
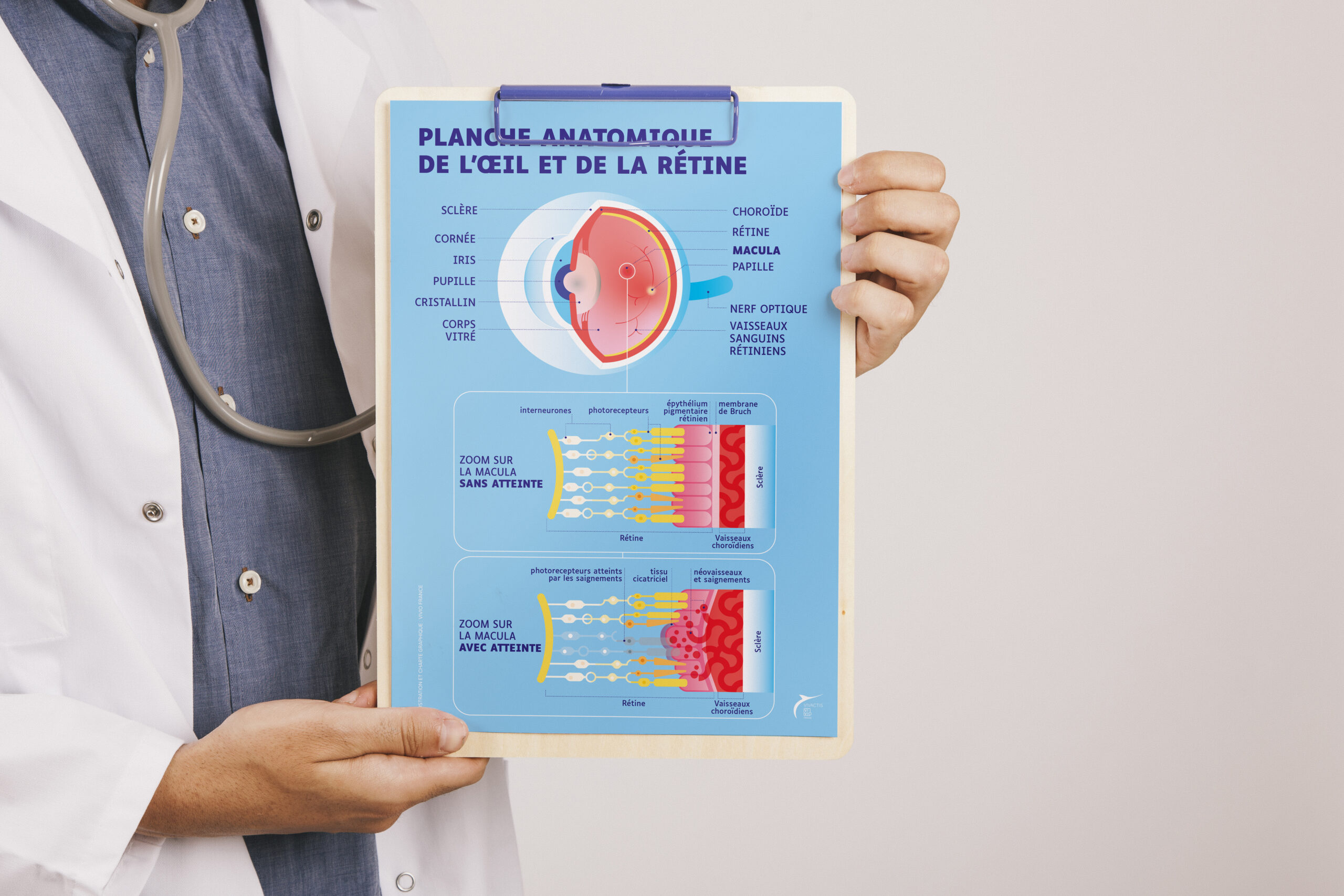
Medical legitimacy (anchored in care centers)
-
Sequenced communication over time
-
Clear distinction between essential treatment knowledge (“CURE”)
and long-term life support content (“CARE”) -
Hybrid formats (print, digital, in-person sessions) adapted to senior users
The project contributed to two scientific publications and helped align healthcare professionals and stakeholders around a more human-centered approach.